New method for diagnosing malaria
Danish researchers have developed a new and sensitive method that makes it possible to diagnose malaria from a single drop of blood or saliva. The method might eventually be used in low-resource areas without the need for specially trained personnel, expensive equipment, clean water or electricity. With the development of this method, the researchers hope to go one step further in identifying and treating all patients suffering from malaria.

Malaria – a global health problem
Malaria is a life-threatening disease that strikes more than 200 million people every year – mainly in Africa, Asia and Latin America. The disease is caused by the Plasmodium parasite, which is spread by infected mosquito bites. Today, malaria can be prevented and successfully treated, but more than half a million people nevertheless die every year from the disease.
Large-scale monitoring and treatment programmes during the past decade have reduced the distribution of the disease, and the frequency of actual epidemics has fallen. However, the number of malaria patients with relatively low infection counts has increased, and the need for more sensitive methods to diagnose the disease has thus increased dramatically.
Development of new, simple and sensitive method
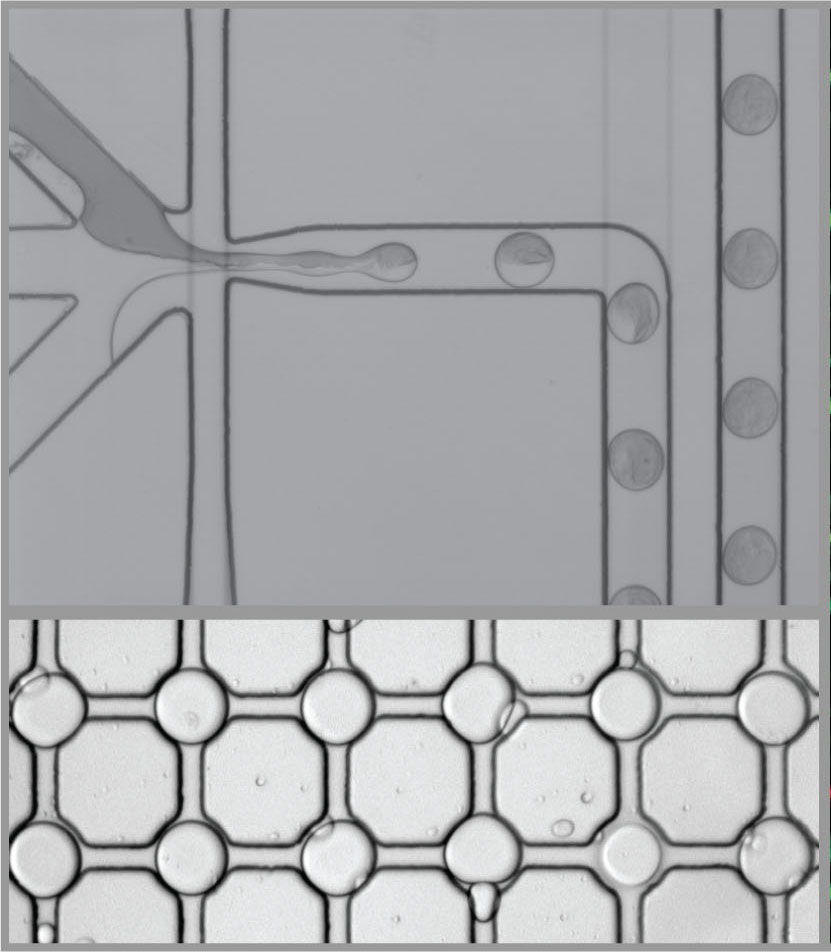
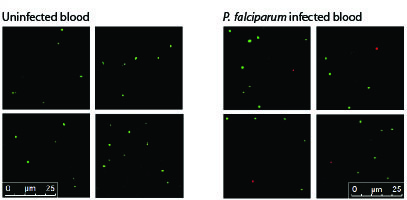
To meet this need, researchers at Aarhus University have developed a new method that can diagnose malaria infections with very high sensitivity. The method is based on measuring the activity of an enzyme called topoisomerase I from the Plasmodium parasite.
The researchers have developed a technology called REEAD (Rolling Circle-Enhanced Enzyme Activity Detection) – which makes it possible to diagnose malaria from a single drop of blood or saliva. This method is much more time-effective and cost-effective than current diagnostic methods, and can be performed by personnel who have no specialised training. It can therefore be used in low-resource areas without the use of expensive equipment, clean water or electricity.
The ongoing fight against malaria is complicated by increasing problems with resistant Plasmodium parasites. In addition, several Plasmodium species (P. vivax and P. knowlesi) cannot be detected with the usual quick-test methods.
The new REEAD-based method distinguishes itself from other quick-test methods because it can measure whether a given Plasmodium infection is resistant to drugs. The newly developed technology is also the only quick-test method that makes it possible to diagnose the less common malaria parasites (P. ovale, P. knowlesi and P. malariae) in addition to the most common Plasmodium parasites (P. falciparum and P. vivax).
The unique sensitivity, combined with its ability to detect infection in very small samples of blood or saliva, makes the method suitable for large-scale screening projects. This is of great importance in areas where the disease is close to being eradicated, and where it is therefore essential to identify and treat all patients infected with one of the above-mentioned parasites – even those who do not show symptoms of the disease.
Interdisciplinary, international collaboration
“This combination of molecular biologists, doctors, engineers and statisticians has been important for our success in developing the new method,” says Associate Professor Birgitta Knudsen, who is the driving force behind the project.
In addition to her group, which is affiliated with the Interdisciplinary Nanoscience Centre (iNANO) and the Department of Molecular Biology and Genetics, Aarhus University, researchers from both Denmark (Department of Pathology and Department of Clinical Medicine, Aarhus University Hospital) and abroad (Duke University, University of Rome, University of St Andrews and University of Lyon) contributed to this project.
- More information about malaria.
- Read the scientific article: Droplet Microfluidics Platform for Highly Sensitive and Quantitative Detection of Malaria-Causing Plasmodium Parasites Based on Enzyme Activity Measurement.
- Zymonostics ApS - a pan-malaria point-of-care test - the new paradigme for malaria diagnosis.
For more information, please contact
Associate Professor Birgitta R. Knudsen
Department of Molecular Biology and Genetics and
Interdisciplinary Nanoscience Centre (iNANO)
Aarhus University
Denmark
brk@mb.au.dk – +45 6020 2673
Text: Rikke Frøhlich and Lisbeth Heilesen
Translation into English: Lisbeth Heilesen
